Project Overview
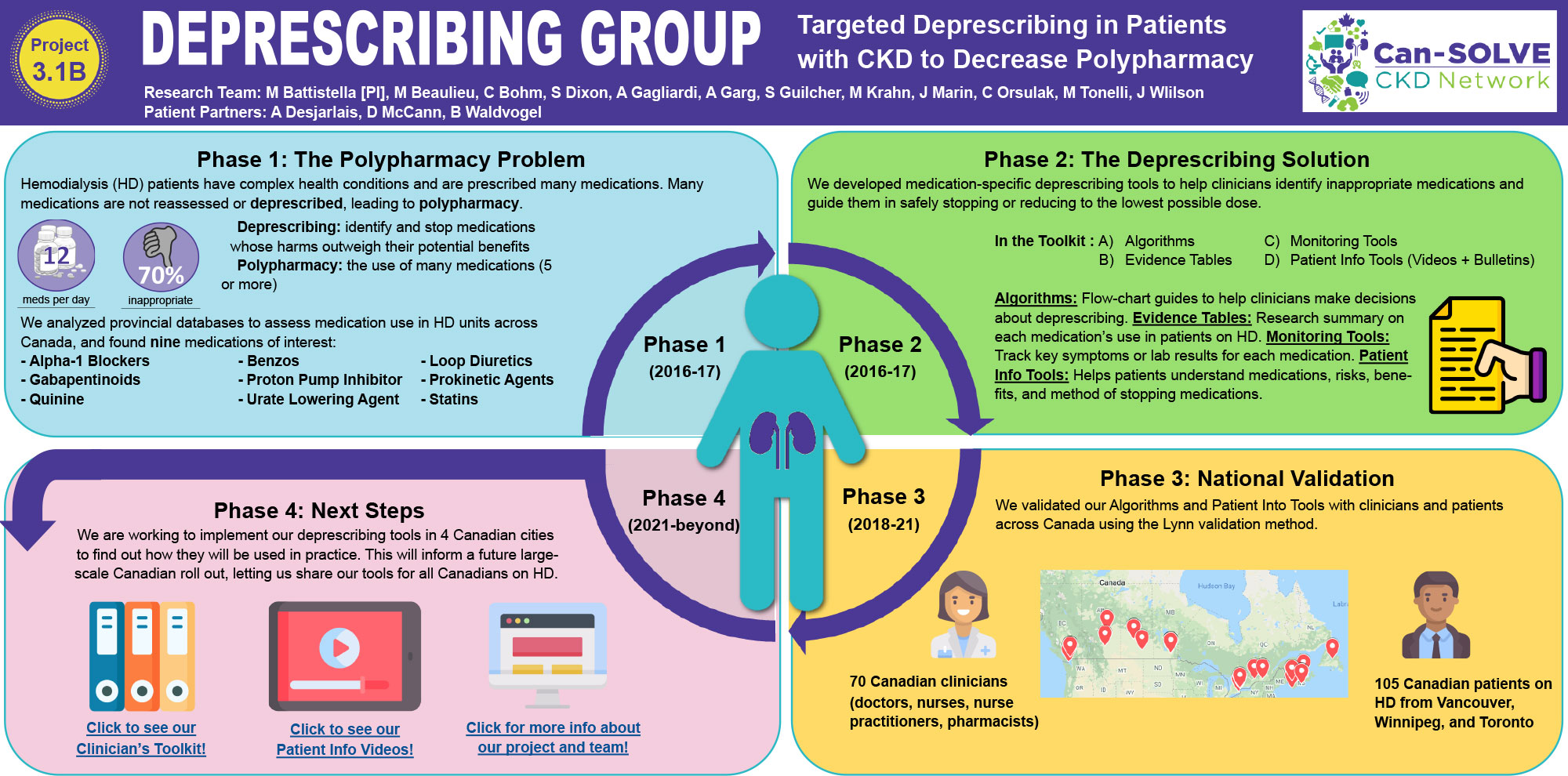
Patients on hemodialysis (HD) take 12 medications per day on average. Many of these medications lack high-quality evidence to show their effectiveness and safety in HD patients. Deprescribing tools have been developed to reduce the use of unnecessary medications and have been successful in the elderly population. We have conducted a pilot study using a deprescribing tool in our HD unit. In our study, we were able to deprescribe medications in 77% of patients and found that more than 80% of medications were being used inappropriately.
This project will develop tools to help reduce the use of medications that lack evidence for effectiveness and safety in HD patients. Our first objective will be to identify a list of potential medications to deprescribe. By analyzing provincial databases, our research group will assess the use of inappropriate medications in HD patients. Using the results, our group will develop medication-specific deprescribing algorithms. Our last objective will be to validate these algorithms using a national consensus method called a modified Delphi approach. These national consensus-driven medication deprescribing algorithms will then be put into use in hemodialysis units across Canada. The goal of these algorithms will be to reduce the use of unnecessary medications and all the associated negative outcomes.
Impact Stories
Finding the right medicine for better kidney health
A Can-SOLVE CKD research project has developed a new tool to help care teams identify unnecessary medications being taken by hemodialysis patients.
Publications
Clinical Journal of the American Society of Nephrology
Battistella M, Ng P
Research Project: STOP Med-HD
Keywords: Deprescribing, Polypharmacy
Development and Validation of Nine Deprescribing Algorithms for Patients on Hemodialysis to Decrease Polypharmacy
Canadian Journal of Kidney Health and Disease
Lefebvre MJ, Ng PCK, Desjarlais A, McCann D, Waldvogel B, Tonelli M, Garg AX, Wilson JA, Beaulieu M, Marin J, Orsulak C, Lloyd A, McIntyre C, Feldberg J, Bohm C, Battistella M
Research Project: STOP Med-HD
Keywords: Deprescribing, Hemodialysis
Connect with us!
Subscribe to receive updates from the Can-SOLVE CKD Network. Learn more about what we do, why it matters, and how you can get involved!